Current Need
The evaluation of urine output has yet to be fully automated in a cost-effective, accurate way. Due to the nature of receiving and analyzing a urine sample, this important task can be time and effort intensive for both nurses and lab technicians. An electronic system for monitoring patient urine output would play a huge role in freeing time for more direct and impactful patient contact by medical professionals and more meaningful analysis to be performed by technicians. In addition, current medical practices have nurses or orderlies measure the volume of patient’s urine after pre-defined intervals (typically 30 minutes to an hour). This method means that real time data of a patient's urine output is not collected, preventing closer analyses of a patient’s kidney health. Electronic monitoring overcomes this by providing accurate measurement over the actual time interval instead of pre-defined intervals. Thus, instead of rough estimates of flow rate, exact calculation of flow rate can be performed.
Project Scope and Design Specifications
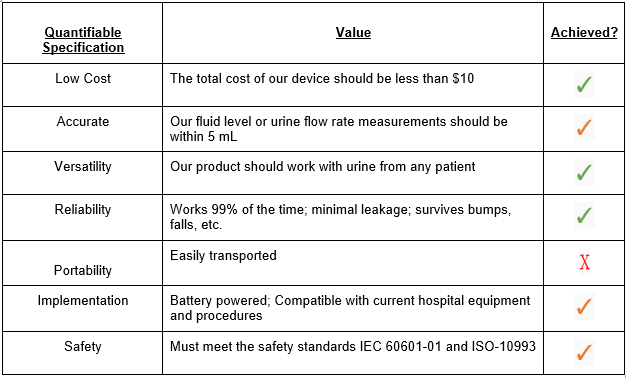
An electronic urine meter has the potential to drastically reduce workload on nurses as well as provide a direct and immediate reading of urinary output. The goal of this project is to develop a device that can accurately measure and display the flow rate of urine from a patient. The following are specifications for our design and if these metrics were met with our proof of concept:
Proof of Concept
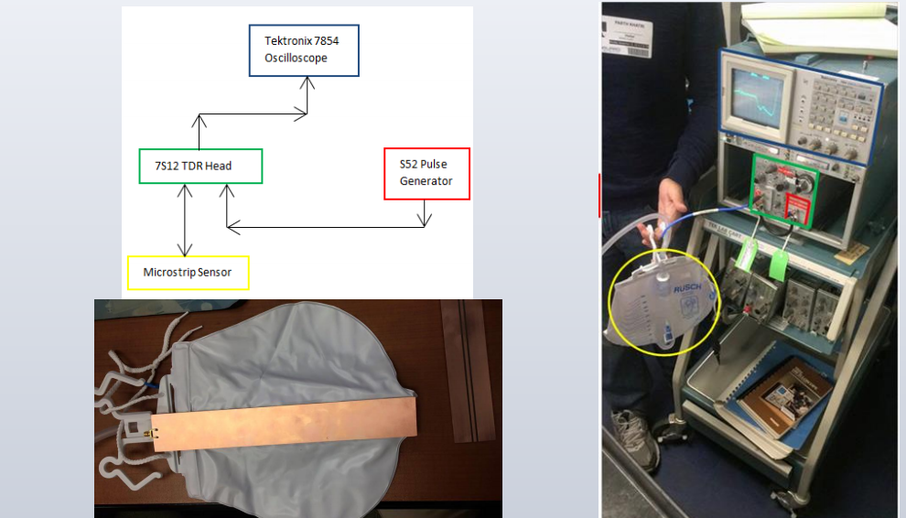
Due to time constraints, we were only able to build a proof of concept as opposed to a full-fledged prototype. We attached a microstrip sensor to the back of a standard urine bag to act as our probe and connected that wire to both a pulser and an oscilloscope. Just as the name suggests, the pulser sends low amplitude, high frequency pulses down the microstrip sensor, which then return to the oscilloscope to output the reflected signal. The signal processor/output/display is missing currently because it would take too long to program a method of exporting the oscilloscope data to a signal processor due to the outdated equipment we are presently using.
Feasibility
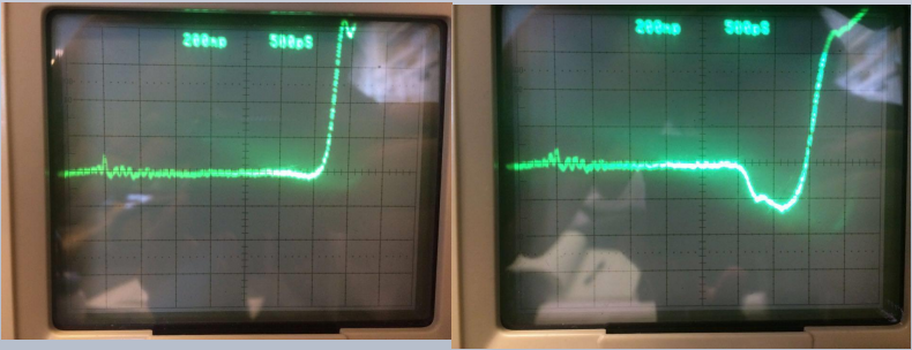
Using a Tektronix 7854 Oscilloscope and changing volumes of water, we were able to show that adding water to the urine bag causes a substantial decline in the reflection coefficient after the pulse crosses the air/water interface.
Left Image: Oscilloscope reading of an empty urine bag
Right Image: Oscilloscope reading of a urine bag with 60 mL of water
Left Image: Oscilloscope reading of an empty urine bag
Right Image: Oscilloscope reading of a urine bag with 60 mL of water
Design Schedule
This was our design schedule for the semester which produced the above results.
Future Direction
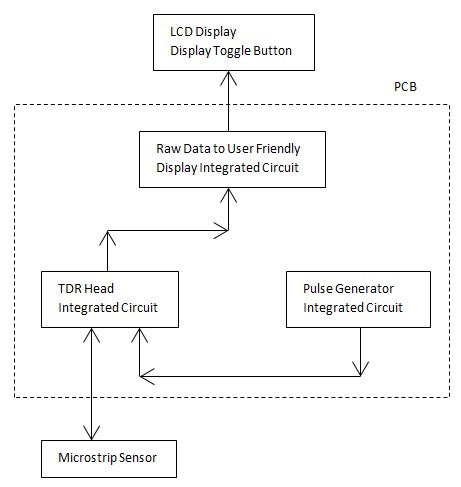
In a product development project, the next step would be to build a fully functional prototype that would implement the flow diagram shown below. This prototype would replace the bulky Tektronix components from our proof of concept.
Additional actions would include the following:
- Pursuit of a provisional patent
- Joining design competitions
- Testing and implementing the product in a clinical setting